Our Hearts Are Heavy: A Parent’s Guide to Understanding and Preventing Aspiration
The news of the sudden and tragic passing of young Umar Shah has left the entire nation heartbroken. As parents, our collective hearts ache for his family. When a child’s life is cut short, it sends a ripple of fear and concern through our community, leaving us with questions and a deep desire to protect our own little ones even more fiercely.
According to reports, the cause was aspiration—a term many of us are tragically hearing for the first time.
At Orange, we believe that knowledge is the first step toward safety. This post is not meant to cause alarm, but to empower you with a clear understanding of what aspiration is and provide practical, simple steps you can take to protect your child.

Understanding Aspiration: What Every Parent Should Know
Imagine our body has two main “pipes” in the throat:
- The Food Pipe (Esophagus): This pipe leads to the stomach.
- The Windpipe (Trachea): This pipe leads to the lungs.
Normally, a small flap of tissue called the epiglottis acts like a traffic controller, covering the windpipe whenever we swallow. This ensures food, liquid, and saliva go down the correct pipe to the stomach.
Aspiration happens when this system fails, and stomach contents (like vomit or reflux), food, or liquid accidentally enter the windpipe and go into the lungs instead of the stomach.
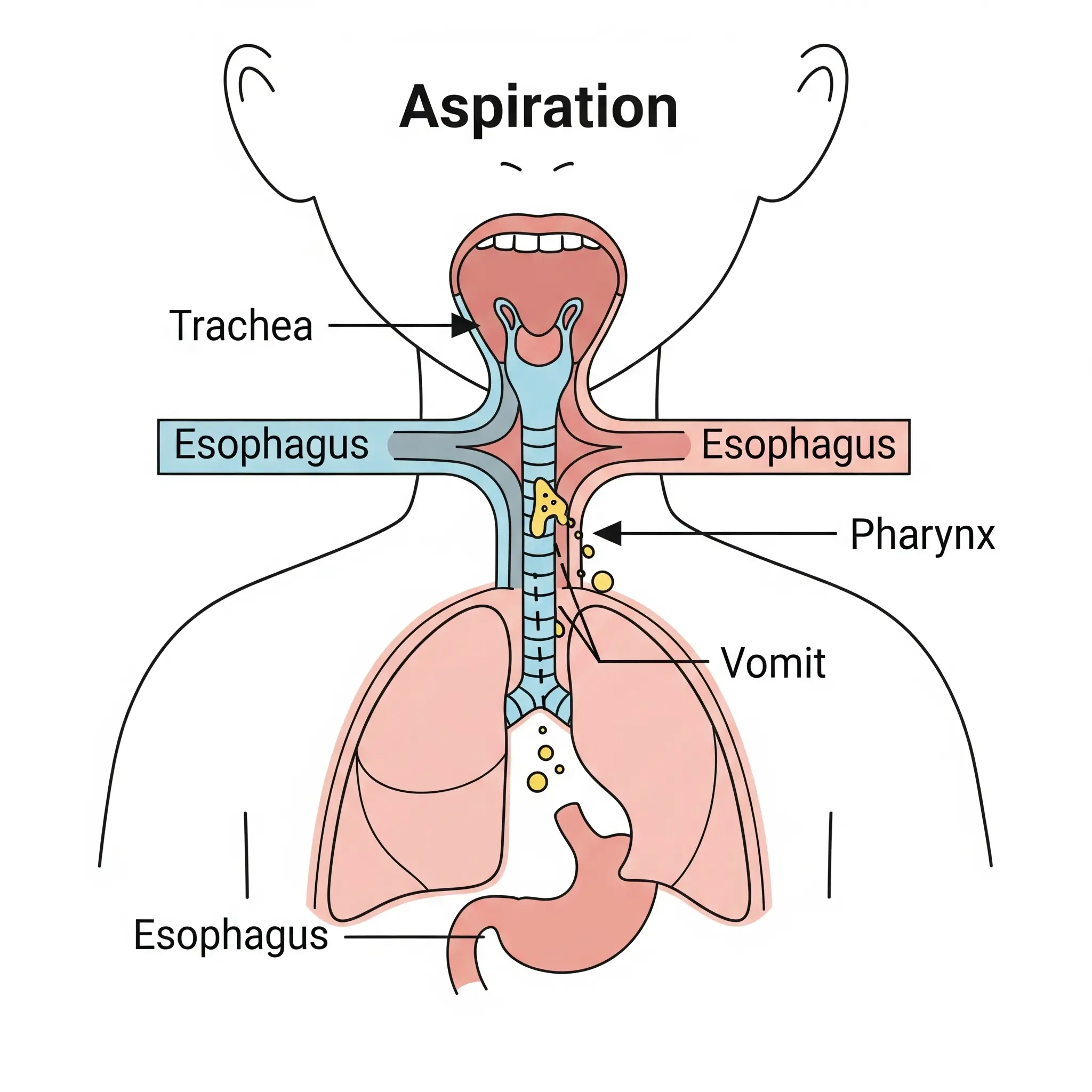
Why is this so dangerous?
When foreign material enters the lungs, it can cause two immediate and life-threatening problems:
- Blockage: It can physically block the airways, making it impossible to breathe. This cuts off oxygen to the brain and body.
- Inflammation: The lungs can become severely inflamed or infected (a condition called aspiration pneumonia) from the acidic stomach contents.
As we saw in the heartbreaking case of Umar Shah, if the airway is significantly blocked, it can cut off oxygen supply and lead to cardiac arrest within minutes.
Why Are Babies and Young Children More Vulnerable?
Children, especially infants, are more at risk for a few key reasons:
- Immature Reflexes: Their swallowing and gag reflexes are not yet fully developed.
- Positioning: They spend a lot of time lying on their backs.
- Common Illnesses: Conditions like acid reflux (GERD) and stomach bugs that cause vomiting are common in children.
Practical Steps to Keep Your Child Safe: Prevention is Key
Knowing the risks allows us to build a fortress of safe habits around our children. Here are the most important steps you can take.
1. Safe Feeding Practices
Whether you are breastfeeding or bottle-feeding, ensure your baby is positioned with their head higher than their stomach. Avoid feeding them while they are lying completely flat. For older children, ensure they are sitting upright while eating and drinking.
2. Promote Safe Eating Habits (For ALL Ages)
- Encourage children to always sit down at a table to eat.
- Teach them not to talk with a full mouth and to chew their food thoroughly before swallowing.
- Make a simple rule: no eating while walking, running, playing, or lying down watching a screen.
3. Burping is Not Optional
Always burp your baby during and after feedings. This releases trapped air that can otherwise come up with spit-up, increasing the risk of aspiration.
4. Critical Care During Illness (For ALL Ages)
This is the most important takeaway for parents of children of any age. When your child is sick and vomiting:
- If they are lying down when they vomit, you must act immediately. Gently and quickly turn them onto their side.
- This position, often called the recovery position, uses gravity to help vomit, phlegm, and other fluids drain out of the mouth instead of down the windpipe.
- Never give medicine to a child who is lying flat on their back, especially if they are drowsy or nauseous. Prop them up first.
5. The 30-Minute Upright Rule
After feeding, keep your baby in an upright position for at least 20-30 minutes. You can hold them over your shoulder or place them in a baby seat. This lets gravity help keep the stomach contents down.
6. “Back to Sleep” is Safest
Always place your baby on their back to sleep, on a firm mattress with no loose blankets, pillows, or toys. This is the safest position to prevent both SIDS and aspiration. If they spit up, their natural reflexes will help them turn their head to clear their airway.
7. Care During Illness
If your child is sick and vomiting, be extra vigilant. Do not give them medicine or fluids while they are lying flat on their back. If they are vomiting while lying down, gently and immediately turn them onto their side. This helps the vomit drain out of their mouth instead of going down their windpipe.
8. Supervise Mealtimes for Toddlers
For children eating solid foods, always supervise them. Ensure they take small bites, chew their food thoroughly, and don’t eat while running or playing. Cut foods like grapes and hot dogs into small, manageable pieces.
Recognizing the Warning Signs
Know what to look for. Seek immediate medical help if your child shows any of these signs, especially during or after feeding:
- Coughing, gagging, or choking.
- Wheezing or noisy breathing.
- Difficulty breathing or breathing that seems too fast.
- A bluish tint to the skin, lips, or nails (cyanosis).
- A weak cry or hoarse voice.
Our Promise to Our Community
Parenting is a journey of love, joy, and constant learning. Tragedies like this remind us of the fragility of life and the importance of community support. By sharing this vital information, we hope to arm parents with the knowledge needed to create the safest possible environment for their children.
Let’s honor the memory of little Umar by holding our own children a little tighter and sharing life-saving knowledge with every parent we know. 🧡
Disclaimer: This blog post is for informational purposes only and does not constitute medical advice. Please consult with a pediatrician or qualified healthcare provider for any health concerns.